Penile prostheses in Windsor & Berkshire
Penile prostheses were first developed over 30 years ago and despite significant advances in the pharmacotherapy for erectile dysfunction (ED), prosthetic surgery continues to occupy an important therapeutic role and 1% of all patients with ED eventually have a penile prosthesis inserted. This equates to 25 000 penile prostheses implanted annually worldwide. Only surgeons who have had very specialised training in andrology perform this operation in the UK.
Indications
- Failure of conservative treatment of ED, including Peyronie’s disease where ED and erectile deformity coexist.
- Penile fibrosis from any cause.
- Early implantation in acute ischaemic priapism refractory to normal conservative measures.
Patient selection
Patients must have realistic expectations resulting from appropriate preoperative counselling. Patient information leaflets and personal handling of prosthetic samples are useful adjuncts.
Ideally the partners of patients should also be involved in the counselling process. Patients must be aware of the serious adverse surgical outcomes of prosthetic surgery. These include
a device infection rate of 2% in patients with no previous surgery and who are not diabetic
and mechanical failure of the device, which occurs with an annual cumulative frequency of 2–
3%. Patients must also appreciate that once a device is implanted any degree of previous natural erection will be lost. Preoperative sepsis, e.g. perineal septic skin lesion or a UTI is a contraindication to implantation.
What does the procedure involve?
This procedure involves insertion of prostheses into the penis to allow a patient to achieve erections for sexual intercourse. The prosthesis may be either a malleable (self-bending) one
or an inflatable one which requires mechanical pump activation. Although not all patients are suitable for both types, this should have been discussed in detail with you before the
procedure. There are currently two inflatable systems on the market the Coloplast Titan
series and the AMS 700 series (Figures 1 and 2).
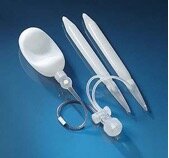
Figure 1. The Coloplast Titan series
The two impant systems are similar but the Coloplast Titan is thicker, which provides more rigidity for men who have a penis length of 7″ and over. The fluid-filled system is made from silicone and Bioflex, a supple, yet durable, biopolymer material. Parts are connected by silicone tubing. The Titan OTR is MRI conditional and latex free. The Titan also features a hydrophilic coating, plus one-touch release (OTR) touch pads for easy, one-handed deflation.
Link to patient video:
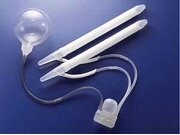
Figure 2. The AMS 700 CX system
The AMS 700 is available in a variety of models and sizes for a custom fit. The AMS 700
Series consists of three models for three different patient types:
700CXTM—Controlled expansion cylinders allow for increased girth; can be used in all patient types that are able to receive a 3-piece prosthesis
700 UltrexTM—For the patient who wants expansion in girth and length; provides up to 20% cylinder elongation.
700 CXRTM—The narrowest proximal profile of any inflatable prosthesis; for scarred, fibrotic or stenotic corpora.
Link to patient Info video:
The procedure
The incision is usually made at the junction of the penis and scrotum. A second incision may be used to insert the balloon reservoir, which is part of the inflatable prosthesis, into the abdomen. Although this can sometimes be done through the first incision, your surgeon may feel it safer to perform this through a separate incision, especially if you have had previous abdominal surgery.
What happens during the procedure?
Either a full general anaesthetic (where you will be asleep throughout the procedure) or a spinal anaesthetic (where you are awake but unable to feel anything from the waist down) will be used. All methods minimise pain; your anaesthetist will explain the pros and cons of each
type of anaesthetic to you.
How long does this operation take?
On average this operation takes 2-3 hours.
Are there any side-effects?
Most procedures have a potential for side-effects. You should be reassured that, although all these complications are well-recognised, the majority of patients do not suffer any problems
after a urological procedure.
Common (greater than 1 in 10)
- Temporary swelling and bruising of the penis and scrotum lasting several days
Occasional (between 1 in 10 and 1 in 50)
- Significant bleeding or infection requiring further treatment which may include removal of all or part of the prosthesis (2-3%)
- Nerve injury with temporary or permanent numbness of the head of the penis
- Drooping of the glans penis requiring correction
- Mechanical failure requiring revision at a later date. This may involve replacement of all or part of the device and can happen at any stage, from a few months to several years later
- Self-inflation due to mechanical failure
Rare (less than 1 in 50)
- Injury to the bowel or bladder during insertion of the balloon component within the abdomen
- Erosion of the prosthesis where a part of the device may break out of its normal position and appear in another site
What are the alternatives to this procedure?
Although surgery is reserved for patients who have tried other treatments, you should discuss the merits of any treatments which you may not have tried with your surgeon. You may not
be suitable for certain treatment as a result of specific medical factors.
How much pain can I expect?
You may experience discomfort for a few days after the proecdure but painkillers will be given to you to take home. Absorbable stitches are normally used which do not require removal.
What should I expect before the procedure?
A week or so before your surgery you will be asked to attend the pre assessment clinic. This clinic is used to check that you are fit for a general anaestheisia and to give you more
information about your hosptial stay and fasting times before your operatiion. You may have blood tests taken and a urine specimen will be required. Depending on your medical history,
you may need an ECG (electrical recording of your heart).
What happens immediately after the procedure?
If an inflatable prosthesis has been used, it is usually left in a semi- inflated position overnight to reduce the risk of bleeding but will be deflated before you are discharged home. You may
experience discomfort for a few days after the procedure but painkillers will be given to you to take home. Absorbable stitches are normally used which do not require removal.
A catheter is usually inserted into the bladder for 24-48 hours after the operation to prevent any problems with passing urine. Once the catheter has been removed and you are passing urine normally, you will be able to go home. Sometimes a drain is used temporarily (overnight) to prevent any collection of blood at the operation site.
The average hospital stay is 1-2 nights after surgery. When you are discharged, you will be asked not to inflate the prosthesis until an outpatient appointment at 2 weeks where we will teach you inflate and deflate it (this is known as “cycling” the prosthesis). Sexual intercourse should be avoided for at least 6 weeks after the operation.
What should I expect when I get home?
By the time of your discharge from hospital, you should:
- be given advice about your recovery at home
- ask when to resume normal activities such as work, exercise, driving, housework and sexual intimacy
- ask for a contact number if you have any concerns once you return home
- ask when your follow-up will be and who will do this (the hospital)
It will be at least 14 days before healing occurs and you may return to work when you are comfortable and your GP is satisfied with your progress. You should refrain from sexual intercourse for a minimum of 6 weeks to allow complete healing.
What else should I look out for?
There will be marked swelling of the penis and scrotum after a few days. This may last up to
10 days and will then subside but do not be alarmed because it is expected.
If you develop a temperature, increased redness, throbbing or drainage at the site of the operation, please contact the hospital or your GP.
Are there any other important points?
A follow-up appointment will be arranged approximately 2 weeks after the operation. You will receive this appointment either whilst you are on the ward or shortly after you get home.
For further information
If you have any further queries or concerns and you would like to discuss regarding this surgery please do not hesitate to contact Mr Jas Kalsi on (01753 665415).
References
- Outcome of penile prosthesis implantation for treating erectile dysfunction: experience with
504 procedures. Minervini A, Kalsi JS, Ralph DJ, Pryor JP. BJU Int. 2006 Jan;97(1):129-33.
- Patient and partner satisfaction after AMS inflatable penile prosthesis implant. Bettocchi C, Palumbo F, Spilotros M, Lucarelli G, Palazzo S, Battaglia M, Selvaggi FP, Ditonno P. J Sex Med. 2010 Jan;7(1 Pt 1):304-9. Epub 2009 Sep 15.
- Satisfaction and complications with the Titan® one-touch release penile implant. Lindeborg
L1, Fode M, Fahrenkrug L, Sønksen JScand J Urol. 2014 Feb;48(1):105-9. doi:
10.3109/21681805.2013.808695. Epub 2013 Jul 8.
- The management of low-flow priapism with the immediate insertion of a penile prosthesis. Rees RW, Kalsi JS, Minhas S, Peters J, Kell P, Ralph DJ. BJU Int. 2002 Dec;90(9):893-7.
- A questionnaire for the evaluation of quality of life after penile prosthesis implant: quality of life and sexuality with penile prosthesis (QoLSPP): to what extent does the implant affect
the patient’s life? Caraceni E1, Utizi L. J Sex Med. 2014 Apr;11(4):1005-12. doi:0.1111/jsm.12453. Epub 2014 Feb 18.
- Long term patient satisfaction and quality of life with AMS700CX inflatable penile prosthesis. Vitarelli A1, Divenuto L, Fortunato F, Falco A, Pagliarulo V, Antonini G, Gentile
V, Sciarra A, Salciccia S, Sansalone S, Di Placido MR, Garaffa G, Pagliarulo A. Arch Ital Urol
Androl. 2013 Sep 26;85(3):133-7. doi: 10.4081/aiua.2013.3.133.










